Vaccines, variants and a third wave

For the first time in weeks, Nepal recorded more than 3,000 new cases on 20 July. There were 25 deaths. The country is on the tail end of what has been a deadly second wave, but the rate of decline in infections and mortality has stalled.
Public health officials blame it on sudden reopening following two-months of lockdown in which many mingled without masks, low vaccination rate, and minimal testing and tracing.
While some experts say Nepal and India are now safe against another major surge of the Delta variant that was largely responsible for the second wave, others warn of a third wave if safety measures are not enforced.
The Delta mutant is now ravaging Indonesia, and spreading across Europe and North America. And scientists say it has affected mostly countries and regions with low vaccination rates.
“The third wave is a matter of when not if. And if we don’t vaccinate as many people as soon as possible, there will be a continued threat of more dangerous variants, and we will be repeating the whole cycle,” warns Buddha Bansyat, a physician at the Patan Academy of Health Sciences.
So far, Nepal has fully vaccinated 1,158,130 people, 3.6% of its total population. Some 10% Nepalis have received the first dose of either AstraZeneca Covishield, Chinese Sinopharm VeroCell or single-shot Johnson & Johnson jabs.
Another 8 million doses of various Covid-19 vaccines are expected by September – some purchased from China, more doses from COVAX, as well as a direct grant from Japan. This should take the total fully vaccinated population near 20%, which together with antigen positive population could cushion the impact of a possible third wave.
“We have now moved on from vaccinating the elderly and frontline workers to groups less at risk of the Covid-19, and we have more vaccines in the pipeline,” says Shyam Raj Uprety, head of government's Covid Vaccine Strategy. “We have applied to buy 10.5 million more doses of vaccines from the COVAX at a subsidised rate.”

Indian public health experts have projected the third wave to hit that country in late August. What happens in India usually follows in Nepal within 12-13 days, and if that is true this time too, Nepal cannot be unprepared like in March.
“If the vaccination program progresses as smoothly as it is happening now compared to the first two surges, the third wave might not be as significant if it happens at all. By Dasain, a significant chunk of Nepalis should have been vaccinated,” explains Sameer Dixit of Centre for Molecular Dynamics Nepal.
Apart from vaccines, in case of a sudden surge, hospitals need to be ready with sufficient beds and ICUs, oxygen, life-saving medical equipment, drugs and functioning oxygen plants. Hospitals must also prepare their paediatric wards since the third wave could affect a younger population.
Since the peak of the second wave when there were close to 10,000 new cases a day and over 200 daily fatalities, international donors have been supplying essential medical equipment to Nepal.
The Health Ministry received 385 ventilators and 970 oxygen concentrators in May June from various donors. District hospitals at local levels have also received direct supplies from aid agencies. These should be in running condition and on standby instead of being stockpiled in Kathmandu, say doctors interviewed for this report.
With the vaccine supply chain less constrained, there is now a debate about reprioritising the doses and a more strategic distribution of supply. Some experts have suggested a ‘firewall strategy’ wherein densely populated cities are fully vaccinated to reduce transmission, and to revive the economy that will in turn restore jobs.
Equitable vaccination is ideal, but in epidemiological terms inoculating a thinly-spread population is not the best use of limited doses. Inoculating younger adults mean they are less likely to carry the virus and transmit it to children, the largely unvaccinated group. Even within cities, the focus must be on the urban poor in congested areas.
“Moving forward, we must now prioritise crowded cities and highly mobile groups for vaccination to help blunt the effect of another wave and save as many lives as possible,” says Sher Bahadur Pun, a virologist at Teku Hospital.
However, epidemiologist Lhamo Yangchen Sherpa worries that focusing in cities may mean the underserved are neglected. “While reprioritising, our strategy should be such that the supply isn’t misused and the neediest aren’t missed out.”
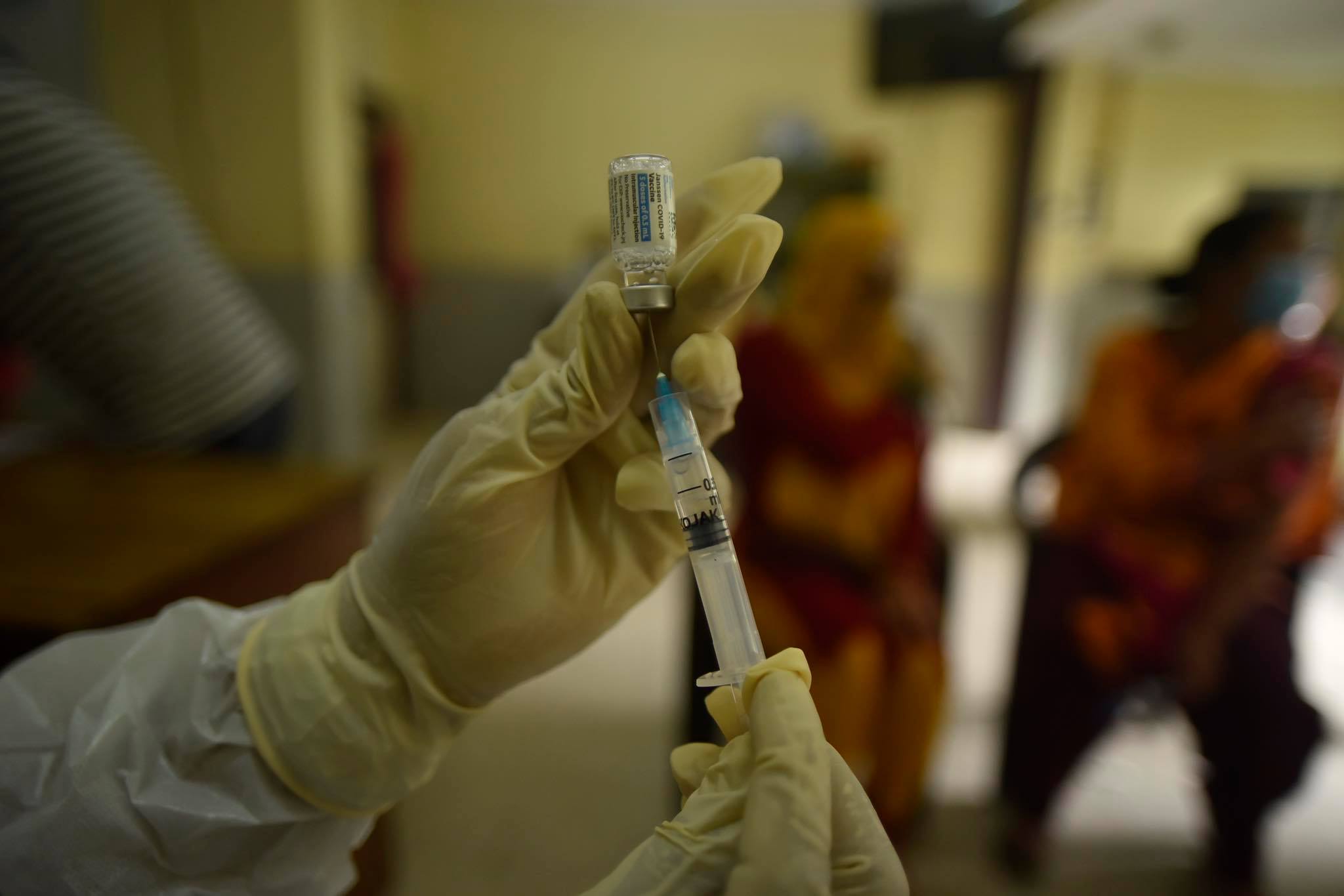
At present VeroCell and J&J vaccination drives are running in parallel across Nepal. Soon, the Japanese grant of 1.4 million AstraZeneca will be used to inoculate the elderly who have been waiting for four months for their second doses.
Social media is rife with speculation about the jabs and who should and shouldn’t get it, leading to widespread confusion and vaccine hesitancy. People are also comparing the efficacy level of one vaccine against the other.
“Let’s take any vaccine available, they do what they are supposed to do, prevent deaths and hospitalisations in most cases,” says Buddha Basnyat. “I encourage people with heart conditions, cancer and liver diseases to vaccinate, they are high-risk group, as well as pregnant women.”
According to Public Health England, Covid-19 vaccines have so far prevented 13,200 deaths and 39,700 hospitalisations in the United Kingdom, even while the country sees a surge in Delta variant cases.
As Nepalis inoculate against SARS-CoV-2, people are starting to forgo safety measures even if the majority of the population remains unvaccinated. They are back on the streets taking part in political rallies and conducting crowded indoor meetings. Jam-packed and poorly- managed vaccination centres could themselves be super spreaders.
Says Sameer Dixit: “In midst of vaccines, variants and new surges, we cannot forget masks and physical distancing, it is still our first line of defence against the coronavirus.”
writer
Sonia Awale is the Editor of Nepali Times where she also serves as the health, science and environment correspondent. She has extensively covered the climate crisis, disaster preparedness, development and public health -- looking at their political and economic interlinkages. Sonia is a graduate of public health, and has a master’s degree in journalism from the University of Hong Kong.




