Nepal tests and treats TB with a flying pharmacy
Ramu Sapkota in Piuthan
Problem: Some 70% of Nepalis are carriers of the tuberculosis bacillus and many of them have full-blown versions of the disease. Although diagnosis and treatment is available, the sick cannot travel to hospitals. How to test the sputum of patients, and deliver antibiotics in remote and road-less parts of Nepal?
Solution: By drones.
Nepal has been acclaimed for its directly observed treatment short course (DOTS) for treating tuberculosis, which demands a combination of antibiotics that are administered under supervision. However, TB is difficult to diagnose and treat in remote parts of this country.
That is why the Britain Nepal Medical Trust (BNMT) is taking a big leap in treating TB with a pilot project in a remote part of Piuthan district in the mountains of central Nepal.
Read also:
TB, Sonia Awale
TB or not TB, Editorial
The Trust has cleverly recycled the DOTS acronym to DrOTS, this time to mean Drone Optimised Therapy System, and is running test flights in the district to collect sputum samples and deliver both diagnoses and treatment to patients living in up-country villages.
The drone flies to health posts in the mountains, and returns sputum samples to the district hospital in Swargadwari Municipality and the public health centre (PHC) in Piuthan Municipality. The samples are tested using a GenExpert kit. If they are positive, patients are given DOTS treatment using smart pill boxes, which keep electronic records of whether or not patients have taken the antibiotics.

“We are using the drones experimentally to ensure that we can reach the hidden cases of tuberculosis, since every untreated patient is a potential carrier of the disease and can spread it,” explains Shraddha Acharya, BNMT coordinator in Piuthan.
During the pilot phase, drones will be used only to collect sputum samples from remote settlements. If the tests are successful, the Trust hopes to use the unmanned craft to also deliver medicine.
Thanks to the initiative, health personnel will no longer need to walk for days to deliver sputum samples from health centres in the villages to the district hospital and PHC for testing, and then return with medicines for those who test positive. The current system results in delays in getting medicines to patients, and also lack of supervision administering the antibiotics.
Read also:
For Nepal, a game-changer in TB control, Buddha Basnyat and Maxine Caws
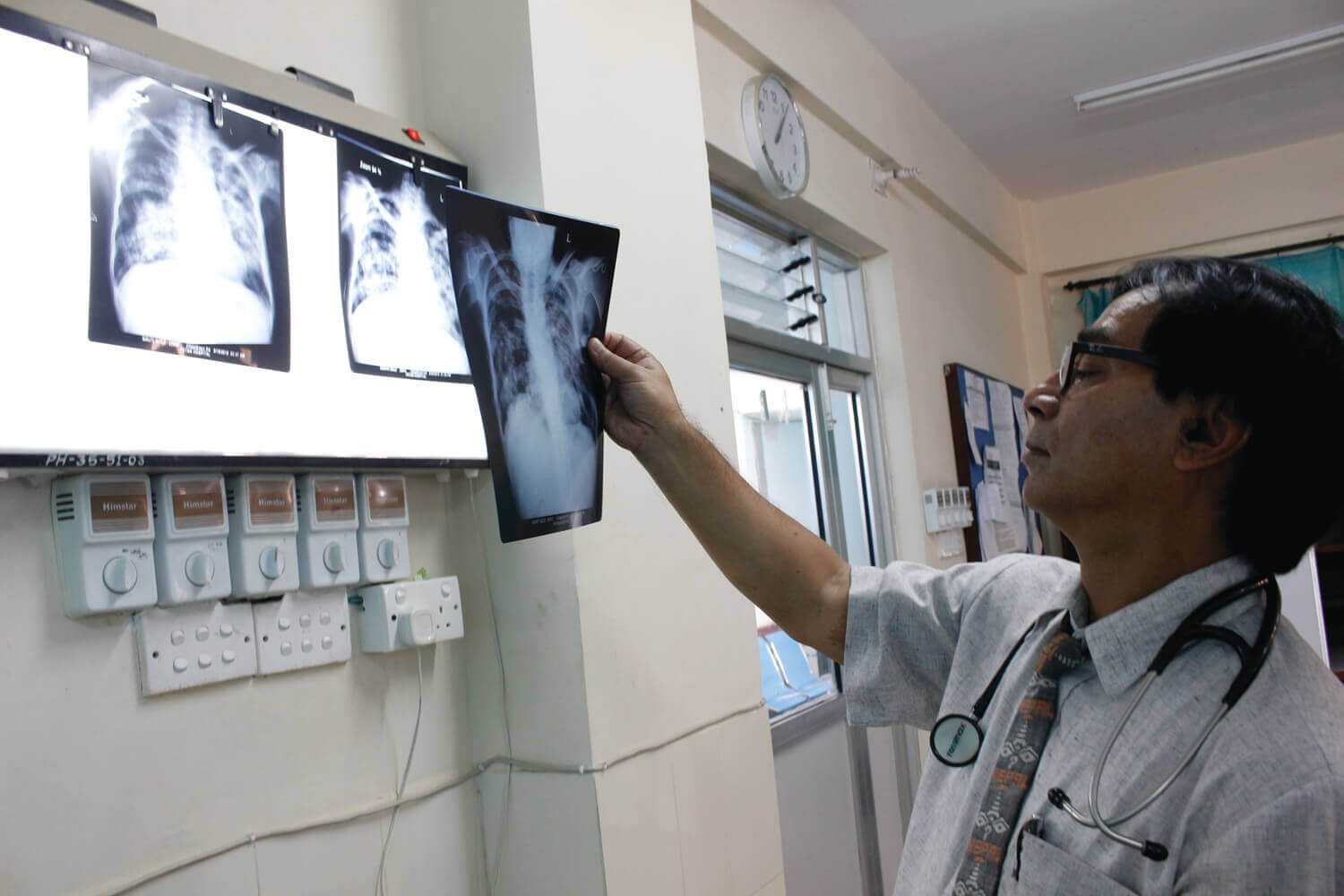
Community Health Worker Sita GC (pictured above) says the drones are god-sent because they can deliver samples in 25 minutes, where earlier it took 2-3 days. “Logistics was a huge problem because of unreliable transport; now it is easy to diagnose and treat quickly,” she adds.

Maxine Caws (pictured above) of BNMT, an epidemiologist with the Liverpool School of Tropical Medicine, says the drones are being tested in Piuthan because it is the mountain district in Nepal with the highest TB prevalence. Last year, the district treated 379 patients for tuberculosis, but 335 new cases were detected in the same period.
The remote-controlled craft are handled by drone specialist Nepal Flying Lab. “We found this to be an exciting project because the drones are ideal for bridging distances to remote areas and the sputum samples and medicines are not too heavy,” says the lab’s Uttam Pudasaini, who adds this is the first time such deliveries are being tested in Asia.
The drones weigh 9kg when empty and can carry another 7kg in a cargo hold designed to protect against biohazards; they can be airborne for 30 minutes. The craft flies at speeds of up to 1km per minute, and is controlled by a pilot at the takeoff point who coordinates with a health worker at the destination. In future, the project plans to train health workers to fly the drones themselves.



The technology has been used for TB control in Zimbabwe and Papua New Guinea. In Nepal, the pilot project is funded by the Nick Simons Institute till December. “Further extension will be determined by whether it is successful and cost-effective,” says Caws.
Sita GC says so far up to 35 positive cases of TB have been detected from sputum samples in Piuthan this month. However, many people refuse to give samples, and others do not follow instructions on taking antibiotics.
The ministry of health is also involved in the drone trials. Spokesperson Mahendra Shrestha says that if the tests are successful the government will take over the program and try to replicate it for TB control in other remote areas.
“If this project is successful, Piuthan and Nepal will be famous worldwide. But the biggest challenge is to first make the tests work,” says Shrestha.
TB or not TB
There are 10 million new cases of tuberculosis every year, and the medieval disease still takes the lives of 1.5 million people annually worldwide.
South Asia accounts for 40% of the global TB burden, with over 4 million cases as well as 40% of total fatalities, a third of them patients who succumbed after they failed to respond to treatment. But worsening air pollution, smoking and alcoholism are big risk factors for TB infection in the region.
Some 11 Nepalis die every day from the highly contagious infection.
There are 40,000 new cases of TB here every year, and Nepal also has a very high rate of latent TB infection. Despite antibiotics, it is often difficult to reach patients in underserved parts of the country and Nepal’s harsh terrain makes it hard to access diagnosis and treatment on time. Experts say there is huge under-reporting of cases.
Nepal is a role model in the community-based DOTS (directly observed treatment short course), with its supervised administration of antibiotics to patients. Yet, experts say much more aggressive case detection and an early treatment system should be in place if the country is to meet the UN target of reducing TB mortality by 95% and cutting new cases by 90%, by 2035.
This means developing techniques to reach the poorest in the remotest parts of the country, and also requires increases in Nepal’s TB control budget and prioritising the infection otherwise known as the ‘poor man’s disease’.
MDR (multi-drug resistant) TB is also spreading, as patients develop resistance to commonly used drugs for treatment. The last survey in Nepal showed that among previously treated cases, anti-microbial resistance was found in 15.8% of cases, against the world average of 18%.
Nepal also has the added challenge of an open border with India and migrant workers continue to bring infections home, while many patients from India come to this country for treatment.
The UN General Assembly held its first-ever, high-level meeting on tuberculosis last year to draw attention and generate investment for TB research, treatment and diagnosis. The SAARC TB Centre located in Kathmandu focuses on prevention and control of tuberculosis and TB/HIV co-infection. Research is also needed for non-resistant drugs with shorter regimen.
Sonia Awale
