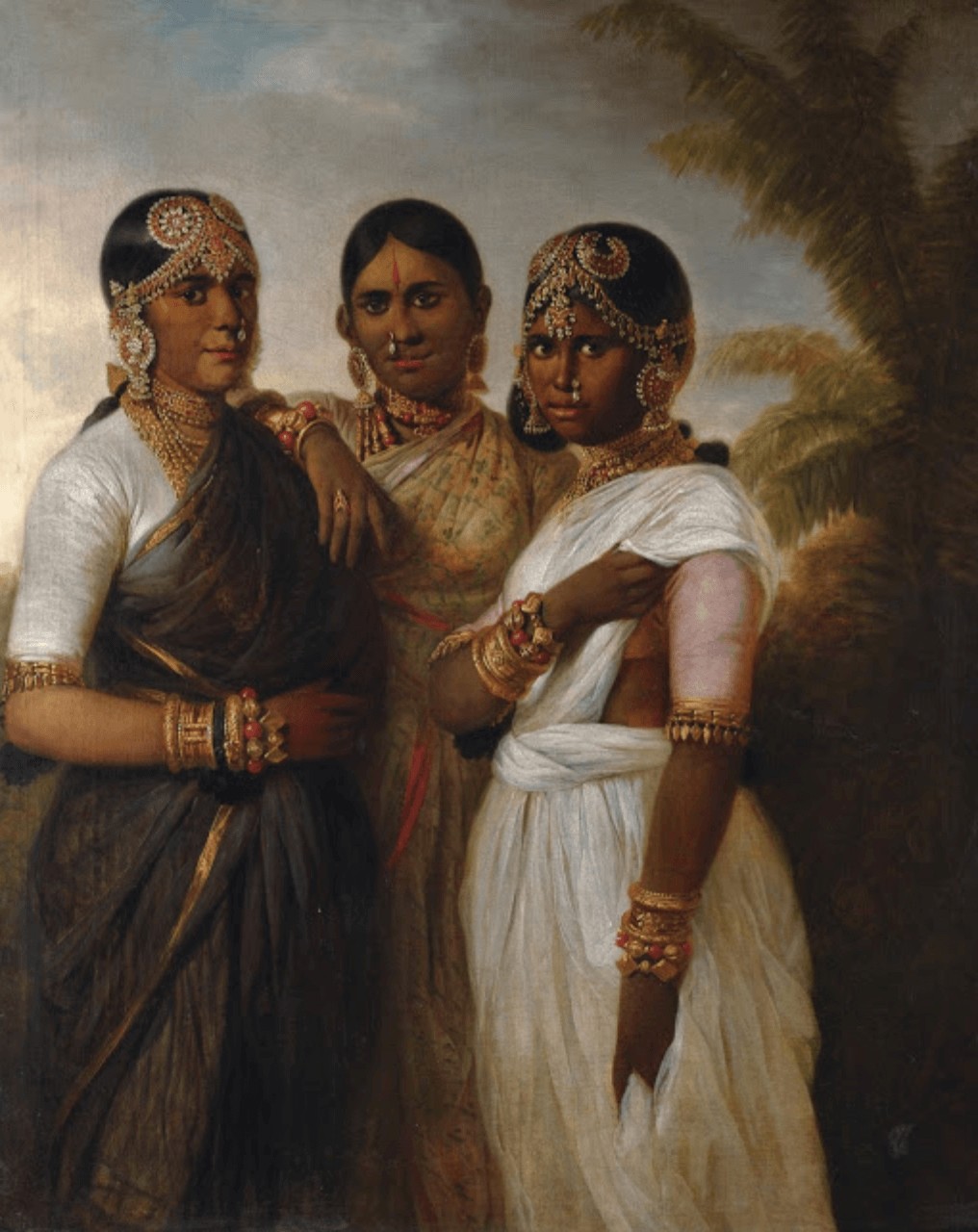
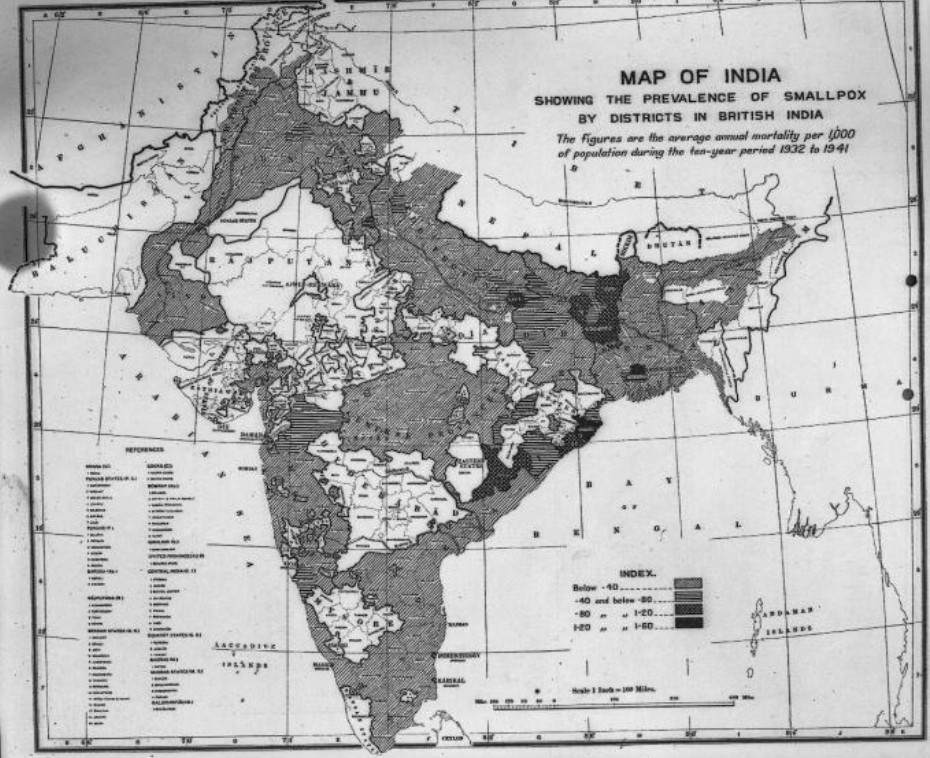
The first record of smallpox in South Asia was in the 7th century, although the virus was probably widespread on the Subcontinent a millennia before that. In late 19th century India, for which we have the first reliable statistics, smallpox struck down more than 100,000 people a year, more in epidemic years. In some parts of north India, few escaped it.
In Nepal, smallpox generally hit in the spring. ‘Transmission reached a peak during April and May,’ a 1977 WHO report notes, ‘and thereafter fell off rapidly as the monsoon increased relative humidity and hampered population movement.’
Smallpox generally attacked children, and older people who hadn't already contracted the disease. ‘Since smallpox erupted epidemically roughly every five to seven years in most parts of India,’ historian of medicine David Arnold explains, ‘its principal victims were children born since the previous epidemic.’
Smallpox was ‘the inevitable bridge which every child has to cross before entering into life,’ noted Sir Sayyid Ahmad Khan in India in 1879. ‘Recovery from the disease is considered second birth.’
Part I: Big story of smallpox in Nepal
Part III: Smallpox, politics and power in Kathmandu
Part IV: How Nepal eradicated the smallpox virus
Part V: Viruses past, present and future
‘It has become quite a saying among the agricultural and even wealthier classes,’ a British planter in the 1860s noted, ‘never to count children as permanent members of the family until they have been attacked with and recovered from smallpox.’
Symptoms did not show during the virus's two-week incubation period. Those infected felt fine, and some even travelled, taking the disease with them, although they were not yet contagious.
But after two weeks, the first of smallpox's horrific symptoms hit: intense fever, often with splitting headaches, body aches, and vomiting. Children often broke into convulsions.
After a couple days, the patient might feel better for a day or two, and even rejoin normal life. But by this point contagious, they risked passing along the infection. Then came a red rash, at first on the tongue but soon all over the body, even on the palms of the hands and the soles of the feet, causing tremendous pain.
By the fifth day, fluid started accumulating in the now bigger and bluish pockmarks. Fever deepened. Eyelids, lips, and nose grew swollen. The afflicted person had trouble swallowing. They might fall into delirium. Lesions could form on the eyes. The patient could be hard to recognise. A dreadful smell was common, as were secondary infections.
At two weeks, scabs formed. They ‘encrust most of the body’, historian Fenn writes. The pain was awful, ‘any movement excruciating.’ The itching could be unbearable. Death, if it was to visit, normally arrived by this point.
The disease also tore apart the lungs, heart, and liver. Smallpox consumed its human hosts ‘as a fire consumes its fuel, leaving spent bodies, dead or immune, behind,’ writes Fenn.
In Nepal, as in much of north India, people thought of smallpox in religious terms, as a visitation by the goddess Sitala, ‘the cool one’. This understanding of disease came with its own remedy: ‘Smallpox was conceptualised,’ historian Arnold writes, ‘not as a disease but rather as a form of divine possession, and the burning fever and pustules that marked her entry into the body demanded ritual rather than therapeutic responses.’
Sufferers showed respect and honour to Sitala with the proper prayers and offerings. 'Oh Mother Sitala,' 19th century Newaris used to sing, 'do not afflict us! Deliver the people, we beg you a thousand times!'
In addition to prayers to Sitala, some South Asians, including Nepalis, used inoculation to head off the disease. They intentionally give their children mild cases of smallpox, hoping that death would not result. Once recovered, the patient would have life-long immunity.
Inoculation carried risks and did not work as well as the vaccine developed from cowpox by Edward Jenner in the 1790s, especially after it was improved during the mid 19th century. But inoculation did save many people from death. Otherwise, smallpox killed one in three of those who got it.
As early as 1802, and for much of the nineteenth century, the British tried to introduce Jenner's vaccine into its Indian colony. But they ran into lots of obstacles, many of their own creation, so it took until the early 20th before vaccinations became common.
What happened? For starters, until the 1850s, the British vaccine was not as effective as they thought, especially in India's heat. Vaccination required person to person contact. Vaccination also cost more than the British wanted to pay, so they did not build the necessary health and education infrastructure.
In addition, cultural gaps surrounding the belief in Sitala, which the British tried to crush instead of to accommodate, also interfered. Many resisted vaccination. ‘To some Hindus,' Arnold explains, 'recourse to any form of prophylaxis or treatment was impious, likely to provoke the goddess and further imperil the child in whose body she currently resided.’
Ultimately, he emphasises, the big problem was that the British administration and medical system in India was‘culturally and politically distant from the lives of its subjects’.
But by the early 20th, the British had improved the vaccine and its delivery, done a better job of explaining its benefits, and begun to meet with more success. In the decade after 1935, for instance, each year roughly 4.3 million people in Madras alone, almost 10% of the population, received vaccinations.
Just as in India, the smallpox virus periodically ravaged Nepal, causing tremendous suffering, killing many, and leaving behind scarring and blindness. It affected all levels of society, even Nepal's royal family on several occasions in the 19th century.
This is the second in a series of articles about the history of disease in Nepal. Forthcoming columns will explore the role of smallpox in Kathmandu’s power struggles in the 19th century, and its eradication campaign in the 1960s. Tom Robertson, PhD, is researching the environmental history of Kathmandu Valley.

