
Only a month ago, even prominent doctors in India were declaring that the country had defeated the novel coronavirus.
They felt that herd immunity in cities like Delhi would protect people from infection and death. Based on a few dubious studies, they conceded that a large proportion of Indians had acquired herd immunity through mild or asymptomatic Covid-19 infections.
Just like the theory that a lifetime exposure to germs would protect South Asians, herd immunity also turned out not to be true.
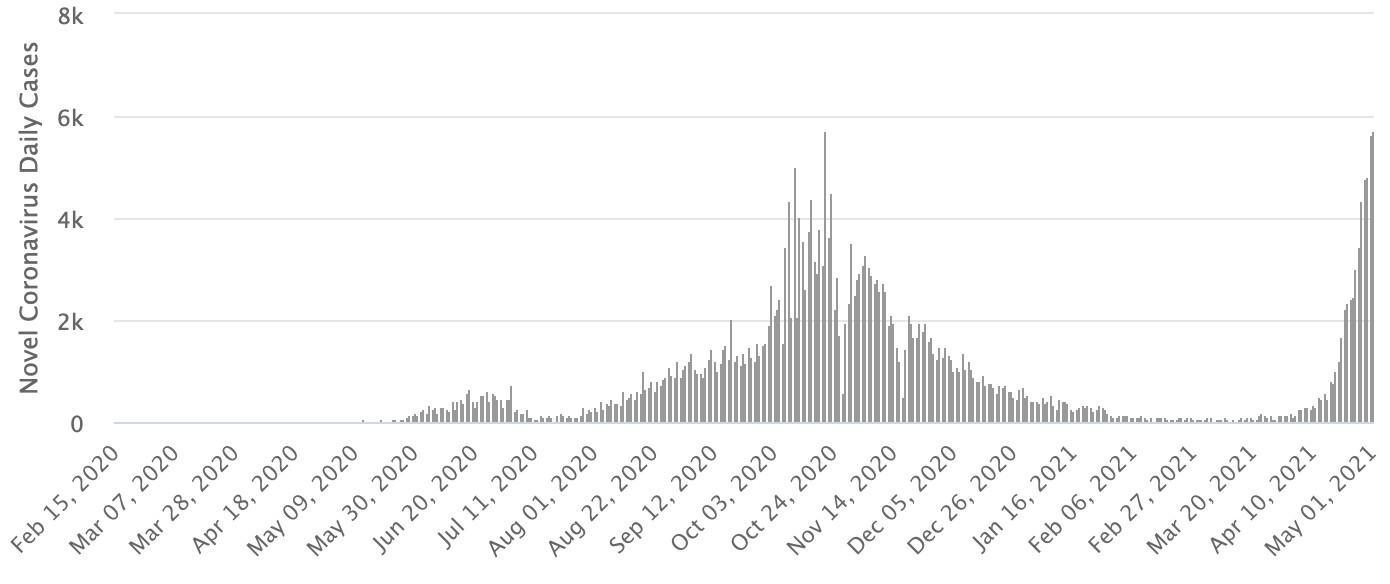
Here in Nepal we are seeing a surge that is proportionately similar to India. The exponential rise in the number of cases, infection of younger cohorts, and the severity of the disease, bear all the hallmarks of the contagion sweeping across India.
While we try to treat the sick by increasing hospital space and ensuring oxygen supply, we must also plan for an exit strategy that entails acquiring more effective herd immunity through mass vaccination, and partial lockdowns enforced with all precautionary measures.
Over-preparation rather than under-preparedness needs to be our mantra. Widespread vaccination is the key to get us out of this pandemic, and we have lost precious time with the delays.
This means our vaccine diplomacy has to go into top gear. If Covishield from India is not available, we must lobby for as many dosages of vaccines from China, Russia, or the United States, and administer them urgently.
All of these vaccines are in general at least 50% effective (the ‘pass mark’ for vaccine efficacy). None of the inoculations appear to have serious adverse effects, even though there are questions about whether they provide enough protection from the new strains, and duration of immunity.
We are trying to immunise the population from SARS-CoV-2, which happens to be a wily killer that exploits the human need for social interaction and mobility. Analysing this sudden and rapid spread of the virus in the Subcontinent, it looks like South Asians are more vulnerable because of our co-morbidities.
South Asians are known to be genetically more susceptible to diabetes and cardio-vascular diseases. The diet and lifestyle of people in the 40-70 age group increases the risk factor for obesity, diabetes and hypertension. Not unsurprisingly, the death toll due to Covid-19 is higher in this age cohort among South Asias than in Europe or the Americas.
The other reason for the infection suddenly taking off again in our part of the world is that we let our guard down, attending festivals, religious ceremonies and political rallies.
And then there is the presence in Nepal of both the UK variant of the virus ( B.1.1.7) and the B.1.617 (Indian variant) both of which are at least 20% more transmissible. The good news (at least so far) is that these variants may not be any more lethal than the standard virus. But even if they are not, we desperately need to stop transmission.
And since this is a respiratory virus, the most effective way to do that is still to wear a mask, avoid crowds and use hand sanitiser.
In a pandemic of this scale, the general public also needs to know what treatment works and does not. Oxygen, if available, is definitely helpful since it is a drop in oxygen level in the blood that leads to serious complications.
A drug called dexamethasone saves lives, it is easily available and cheap. Tocilizumab, unavailable in Nepal, and expensive, can also be used to treat severely ill patients and should only be administered by a physician. There are web links with pragmatic tips that may come in handy if a hospital bed is not available, as we are now seeing in India and Nepal.
There is a lot of fake news about the effectivity of treatment drugs. The following commonly used drugs for well-known illnesses do not work against Covid-19 although, even today, many are rampantly and unnecessarily prescribed in South Asia: Azithromycin, ivermectin, choloroquin, colchicine, convalescent plasma, vitamin D, zinc, lopinavir-ritonavir, favipiravir, and doxycycline.
Even remdesivir, the drug that many desperate families try to acquire for their hospitalised relatives, does not save lives even though it is known to reduce hospital stay.
Many of these drugs were studied for their efficacy by carrying out large randomised controlled trials by the biggest, adaptive Covid-19 tests undertaken by Oxford University’s Recovery Trial.
The Nepal Health Research Council was the first country set-up outside the UK that recently started collaboration with Recovery Trial as part of a global effort to in order to help find a treatment drug against Covid-19.
This tragedy has exposed the inadequacy and inequity in the health care system of Nepal and South Asia. The dominant method of health care delivery in the region, especially for curative services, are private enterprises that follow the corporate health care model patterned after the United States.
Nepal has also increasingly gravitated towards this system of health care, with many new private hospitals all over the country. The pandemic will force us to question this model, and ask if alternatives like the UK National Health Service would be more suitable.
Despite the vested interests behind the medical-industrial complex in Nepal, we need to plan for universal health care (UHC), and even consider universal basic income (UBI), if we are going to improve health care to the vast majority of Nepali people.
Even President Joe Biden is trying to reform US health care with a stimulus package that has clear aspects of UBI. We need to look at a combination of UHC and UBI in Nepal because even if we survive this pandemic, there is certain to be another one sooner or later.
The international media has only taken notice of the second wave in Nepal after reports of infections at Mt Everest Base Camp last week. But it is reassuring to know that even up there at 5,364m, Nepali specialists are doing their best to follow protocols to deal with suspected Covid-19 among climbers and support staff.
This work is critical because the ubiquitous ‘Khumbu cough’ and even the life-threatening high altitude pulmonary edema (HAPE) simulate the symptoms of Covid-19, and it can be difficult to tell them apart.
Buddha Basnyat, MD, is a clinical researcher at the Patan Academy of Health Sciences and an expert in high altitude medicine. He is also a frequent health columnist for Nepali Times.

