This is how to upgrade Nepal's rural health
Bayalpata Hospital represents a functioning model of accessible and affordable medical care in remote Nepal
Sewa Bhattarai in Achham
Deukali Shahi, 26, looks relieved after delivering a healthy baby girl, but her calmness belies her traumatic childbirth. Her eyes fill with tears as she speaks haltingly of the previous baby she lost and the desperation she felt this time to reach the hospital fast enough so this one would live.
Soon, Shahi is overcome with grief and cannot say more. Her sister-in-law Tulaja fills in the rest of the story. The baby was in breech position, but the family did not know this until Deukali was already in labour. They took her to a nearby healthpost, where the nurse said there was nothing they could do. They went on to the district hospital in Mangalsen, which did not have a surgeon to perform a caesarean.
“We drove another four hours and arrived here at two in the night, and the doctors operated on her,” Tulaja said. “Now we have a healthy baby girl.”
Deukali lost her first child due to the same complication, but the family did not know why the baby would not come out. In these remote mountains of Achham, home delivery is the norm and the district has one of the highest maternal mortality rates in Nepal.
Read also: State of the art rural hospital, Marty Logan

All that is changing with Bayalpata Hospital, which serves as the informal referral hospital for Achham and six surrounding districts. The government hospital is managed by the non-profit Possible Health (formerly Nyaya Health) as a private-public-partnership, and now serves 100,000 patients per year.
Bayalpata’s safe motherhood program is accessible at any hour of the day. In the severely understaffed Far West region, Possible is practising an experimental model of healthcare that has become a lifeline for thousands of people in nearby districts. Province 7, which includes Achham, has 13 public hospitals, 16 primary health care centres and 376 health posts, but most of these are under-equipped, under-staffed and under-funded. Aside from government neglect, geography is a further challenge in these mountains. Patients like Deukali have to walk or travel for days to reach a proper hospital like Bayalpata.

The World Health Organiaation recommends a doctor-patient ratio of 1:1,000, and while it is 1:850 in Kathmandu Valley, the rate is 1:150,000 in rural areas. A recent report by the Nepal Government shows that 20% of staff positions in the healthcare system are not filled.
When Nyaya Health took up an abandoned government hospital in Bayalpata 10 years ago, there were no doctors for the people living in the area. The unmet need was so great that the newly-opened hospital could not cope with demand, and soon expanded its facilities. (See box below)
“Nepal’s per capita income is very low, and more than 70% of Nepalis cannot afford private healthcare. So a model like this, which makes healthcare free and accessible, is very necessary in Nepal today,” says Bikash Gauchan, medical director of Bayalpata Hospital.
With grants from the government and donations from philanthropic individuals and organisations, the hospital provides free medical care to up to 500 patients a day, covering a catchment of 230,000 people in Achham’s neighbouring districts.
“The perception in Nepal is that a PPP model is meant to bring in investment for large-scale infrastructure projects like hydropower. When we proposed a model where hospitals would utilise the government funding they deserve, it went against the grain and people found it hard to understand,” says SP Kalaunee, executive director of Nyaya Health Nepal. “But we want to get the best of both worlds: use government funding and resources, but enhance them with our knowledge, skills and management expertise.”
Among many things that make Bayalpata different from the average government hospital is its Integrated Healthcare System, digitising patient records. The software is unique in Nepal and allows the facility to track the health of patients including pregnant women, children under two and those with chronic diseases. Community health workers reach out to these patients door-to-door instead of waiting for them to get so sick that they have to travel to hospital.
“Each of us meets patients in our village once in 1-3 months, as per the need,” says community health worker Dwarika Rawal. “I meet women of reproductive age and talk to them about family planning, tell them about the different methods available. I also check the weight and health of children below 5, and counsel their parents about child health and hygiene.”

Rawal also follows up with patients living with chronic diseases such as diabetes, HIV, TB, high blood pressure and mental disorders, including to see if they are taking their medicines.
In the past decade, health indicators in this region have shown a marked improvement because of Bayalpata Hospital, even surpassing targets in Nepal’s National Health Strategy (NHSS) for 2020 and the UN’s Sustainable Development Goals (SDGs) 2030. In the Sanfebagar area, institutional deliveries have gone up to 96%, compared to the NHSS target of 70% and the SDGs’ 90%. Neonatal mortality has fallen to 6 per 1,000 live births, a third of the NHSS target (18), and half of the SDGs target (12).
Eventually, Possible hopes to not just improve service to its patients, but push through its Integrated Healthcare System, which would make local governments more responsible for providing overall healthcare rather than just operating a particular medical facility.
“What makes our model successful is more accountability, and that is what is needed in our public healthcare system. We do not necessarily need more health facilities, we need to make them functional: make sure that the staff are always available, the medicines are stocked and the equipment functions as it is supposed to,” says Kalaunee. “Public healthcare needs to incorporate the use of technology and outreach to become comprehensive.”
Building a rural hospital from scratch

When a group of Nepali and American public health students set up Nyaya Health and took over an abandoned district hospital in remote Achham district in 2009, there was not a single doctor for over 250,000 people.
Ravaged by government neglect and endemic TB and HIV/AIDS, the region had some of the worst child and maternal mortality rates in Nepal, and the shortest lifespan. Subsistence farmers moved to India to work most of the year so they could support families back home.
Soon, Bayalpata was treating 12,000 people a year out of two rooms, and today it sees 100,000 patients from Achham and six surrounding districts. Renamed Possible, the organisation needed to expand to cater to the huge unmet healthcare demand of Far West Nepal.
Paid for mostly by crowd-funding the $4 million three-phase expansion of Bayalpata Hospital is now complete. Coming round the bend on the highway from Surkhet, the modern facility with its state-of-the-art architecture seems like a mirage in the middle of nowhere.
Today, Bayalpata Regional Hospital is not just unique for its successful model of a private-public-partnership for rural medical care, but also for its distinctive design using rammed earth technology.
An obsolete government facility is now one of the most modern and eco-friendly hospitals in Nepal, providing accessible and affordable health care to the most underserved part of the country.
“Our specs were to use local materials as much as possible, keep energy costs low, and respect the local context,” explains Arun Rimal, a Nepali architect with the US-based Office of Structural Design (OSD). “The rammed earth uses local clay and sand from the river. The thick walls give thermal mass for insulation, and the skylights optimise sunlight and ventilation.”
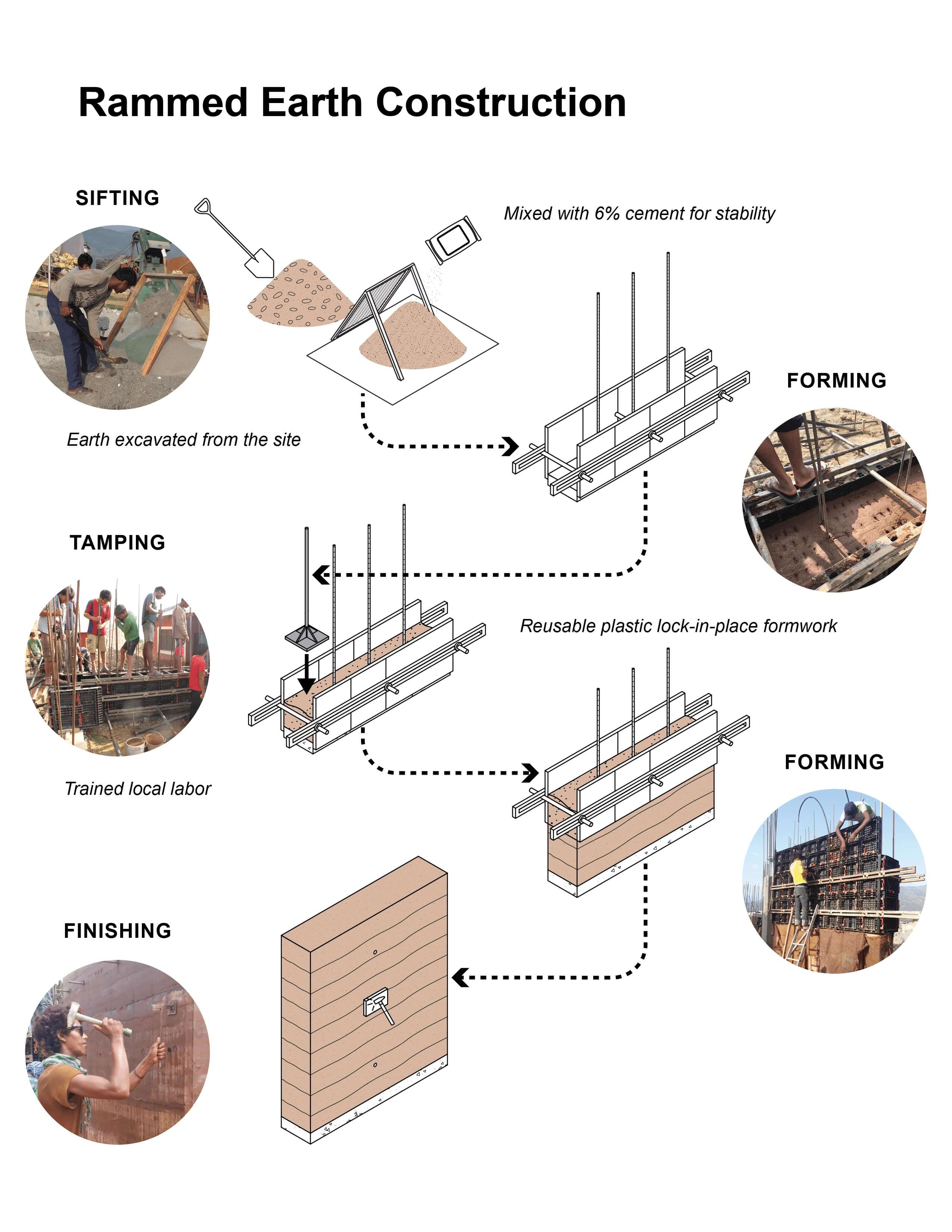
The reliance on local material turned out to be a huge advantage because the project faced unforeseen logistical problems due to the 2015 earthquake and Blockade. However, the four-year construction was delayed by just six months because it did not rely too much on bricks, steel and other imported material.
The facility has a rainwater harvesting system, treats its wastewater and has a network of greywater-irrigated terraces and bioswales to control erosion and recharge the acquifer. A 100kw solar array on the roof meets most of the hospital’s electricity needs, even powering the facility’s only air conditioning unit in the surgical ward.

“It was a deliberate design decision to work with the natural environment as much as possible and also to address the cultural context,” says Tyler Survant from Sharon Davis Design in New York, which also conceptualised the unique Women's Opportunity Centre in Rwanda. “We had to plan for a different kind of hospital from the West: here you have patients and relatives who have travelled for days on foot to get here.”
Bayalpata has public outdoor spaces and canopied courtyards to serve as comfortable waiting areas, while the operating theatres and wards are recessed. Unlike in the US, staff housing also had to be integrated into the facility since it has fulltime resident doctors, who live with their families.
Bayalpata has been shortlisted for the World Architecture Festival 2019, and besides providing vital medical care for much of the Far West, it is sure to become a landmark for sustainability in Nepal’s architectural landscape.
