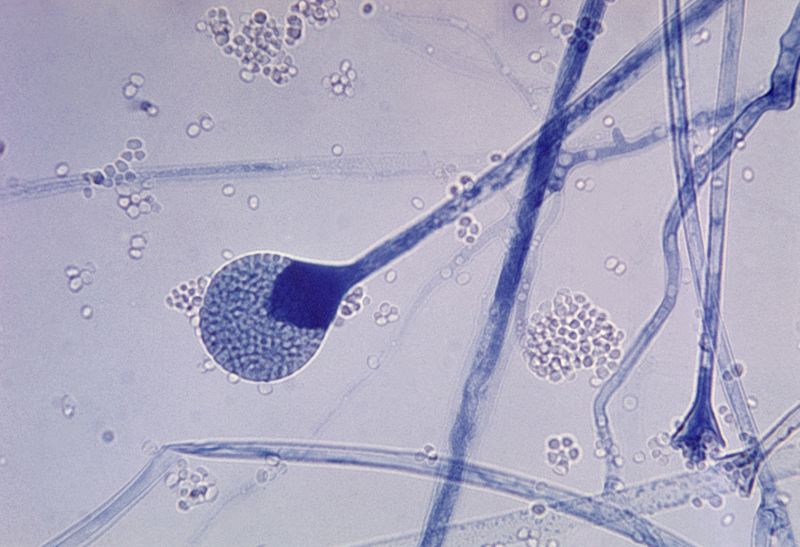
Many public health specialists in Nepal have been heaving a sigh of relief that the infection graph for the second wave is starting to flatten, but with reports of black fungus, third wave and new variants there is no respite.
Everything that India has suffered since March has repeated itself in Nepal on a smaller scale. The black fungus outbreak could be a microcosm of the post-second wave world, of ‘epidemics within a pandemic’ as opportunistic infections and new Covid-19 waves prey on collapsed health systems.
In theory, Nepal should not have a strong flare-up like India because we have fewer risk characteristics, says epidemiologist Lhamo Yangchen Sherpa.
“Covid is communicable so it spreads regardless of demographic factors, but black fungus is rarely contagious and selective.” she says. “India’s population has a higher proportion of elderly, diabetics and immunocompromised people than us, and these are the groups most vulnerable to black fungus,” she says.
Indeed, there were reports in India of black fungus even pre-Covid, with 140 cases per million, which was the highest in the world. It currently has 12,000 cases and 300 deaths from the fungus that mostly affects Covid patients on ventilators and survivors on long-term steroid treatment.
But for all we know, the infection may already spreading in Nepal, starting from the Tarai and moving up just like the Covid second wave. The ‘black fungus’ mucormycosis is found abundantly in the soil, and thrives on steroid overuse, especially on Covid patients with diabetes and other ailments.
Cleared out easily by a healthy body, mucormycosis latches on to patients whose immune systems are compromised.
“Covid treatment is a double-edged sword, it suppresses the virus-induced hyperimmune response but also raises blood sugar levels and weakens infection-fighting ability, making conditions perfect for mucormycosis,” explains Sherpa.
The Health Ministry announced in its daily briefing on Thursday that there were 6,825 new confirmed Covid-19 cases-- up from Wednesday's tally of 5,316--with 5,904 recovering. This brings the total number of active cases to 576,936, with 101,839 in isolation . Of the 1,444 in hospital ICUs, 398 are on ventilator support.
Those in ICUs and ventilators face a double whammy as hospitals treat them with steroids and desperately reuse uncleaned humidifiers and discarded oxygen cylinders. According to the Health Ministry, 10 to 12 patients with black fungus have been detected so far, but there may be more.
Covid survivors who needed critical ICU treatment and are continuing with steroids are left more susceptible to black fungus infection anytime. Nepal’s first recorded fatality from black fungus was a 60-year-old patient in Lumbini Provincial Hospital recently recovered from Covid.
“Black fungus infection has been spotted even in those recovered from Covid for the past six weeks or more,” say Khemraj Bhusal a consultant physician at Greencity Hospital. But as stable survivors are sent home they become potential blind spots in black fungus tallies.
Hospitals in the frontlines can ill-afford to meet new shadow caseloads. Diagnosing mucormycosis infection early requires biopsies, sample examinations and even follow-up CT scans, requiring specialised personnel and advanced equipment that most district hospitals in Nepal do not have.

While manageable if caught on time, the invasive nature of the disease is difficult to treat. In the most common rhinocerebral variety, the fungi eats through subcutaneous tissue and leaves behind characteristic black lesions on the septum and oral cavity. Infected tissues must be removed and eyes even sacrificed to save the brain from lethal infection. If left untreated, the infection has a mortality rate of 50%.
Treatment in such cases involves multiple organs, thus requiring teams of microbiologists, internal medicine specialists, intensivist neurologists, ophthalmologists, dentists and surgeons. But with civil service exams for doctors in limbo for years, rural hospitals lack the specialists necessary to deal with severe cases.
Similar to the pandemic at large, life-saving shots against mucormycosis infection are in short supply.
“Liposomal amphotericin B is an effective treatment, but fungal infections are normally so rare that antifungal production, and therefore supply, is low,” says Associate Professor of Microbiology at Tribhuvan University Megha Raj Banjara.
Amphotericin treatment is extensive, with as many as 60 to 100 vials of injections needed across 4-6 weeks depending on infection severity. In the event of an outbreak, huge stockpiles are needed. Treatment is also costly, with one-day therapy costing upwards of Rs50,000.
Meanwhile, alternative medications like posaconazole and isavuconazole have toxic side effects, are also expensive and less effective.
Imports of amphotericin are the only solution, but as with the pandemic, prospects do not look encouraging. India has already imposed restrictions on amphotericin B export, itself shipping in 200,000 vials from Gilead Sciences in the US, with reports of hoarding and price gouging. Despite warning signs, there has been no appeal for amphotericin shipments from the Nepal government.
If that ws not enough to worry about, India is seeing signs of an early third wave, with 8,000 children infected in a single district in Maharashtra state. With low vaccine penetration in the under-18 cohort, children in Nepal could be next, just like the first two waves.
Meanwhile, 1,350,000 Nepalis above age 55 are set to miss timely booster doses as there is no possibility of securing Covishield shipments from India, according to Chief of Family Welfare Division of the Health Ministry Taranath Pokhrel. He said Nepal is trying to procure the Oxford AstraZeneca from other countries for this cohort, but so far there are no firm deals.
The third wave is set to hit India around July, giving Nepal about a month and half to rush vaccine doses for its vulnerable age groups. Till then, Nepalis will be left once more to fend for themselves. Aggressive self-medication and quack remedies such as cow dung baths are rampant, leaving Covid patients at increased risk of co-infections like black fungus.
“Patients are able to buy medicines without prescriptions from lax pharmacies.” says Sherpa. “Covid patients should avoid self-medication and only medicate under the strict supervision of health professionals or risk being exposed to secondary infections.”
Simple changes can mitigate black fungus. Hospitals should routinely change humidifier water for ventilated patients and avoid sharing oxygen tubes and masks, says Binita Sharma, Chief Medical Director of Netra Jyoti Sangh. She says those with symptoms should immediately get checked up.
To prevent future Covid-19 waves, experts say high-disruption strategies are needed at a time when lockdowns are being relaxed. Ultimately, it will be vaccines and they are needed before the third wave.
