
Going by the Ministry of Health figures, Nepal’s Covid-19 pandemic has peaked, and the number of daily cases, the positivity rate and the number of active cases are all going down.
The recovery rate now exceeds 90%.
Is Nepal turning the corner on the pandemic? Experts say no.
The number of fatalities is at an all-time high. There were 29 deaths reported each on Monday and Tuesday, taking the total to 1,538. And the reason the daily case rate is lower is because the government is conducting fewer tests, there is virtually no official contact tracing, and active cases are at home and going to hospital only when they are really serious. These are ideal conditions for community spread.
“The fact that the fatalities are increasing, especially in Kathmandu, won’t allow us to say that fewer people are getting infected. This coronavirus isn’t going anywhere just yet,” explains Sher Bahadur Pun of the Ministry of Health. “Yes, the positivity rate has gone down, but the government has also more or less stopped contact tracing.”
Since the government started charging for RT PCR tests and hospital admissions, patients and their families are reluctant to have tests despite symptoms, and do not want to go to hospital. The rates have remained high because those infected during Dasain-Tihar are developing symptoms. The current marriage season is another super-spreader event.
There are 77 hospitals and labs across the country conducting an average of 9,000 PCR tests a day, which went down from a daily total of 15,000 after the government directive to charge Rs2,000 for PCR tests in public facilities.
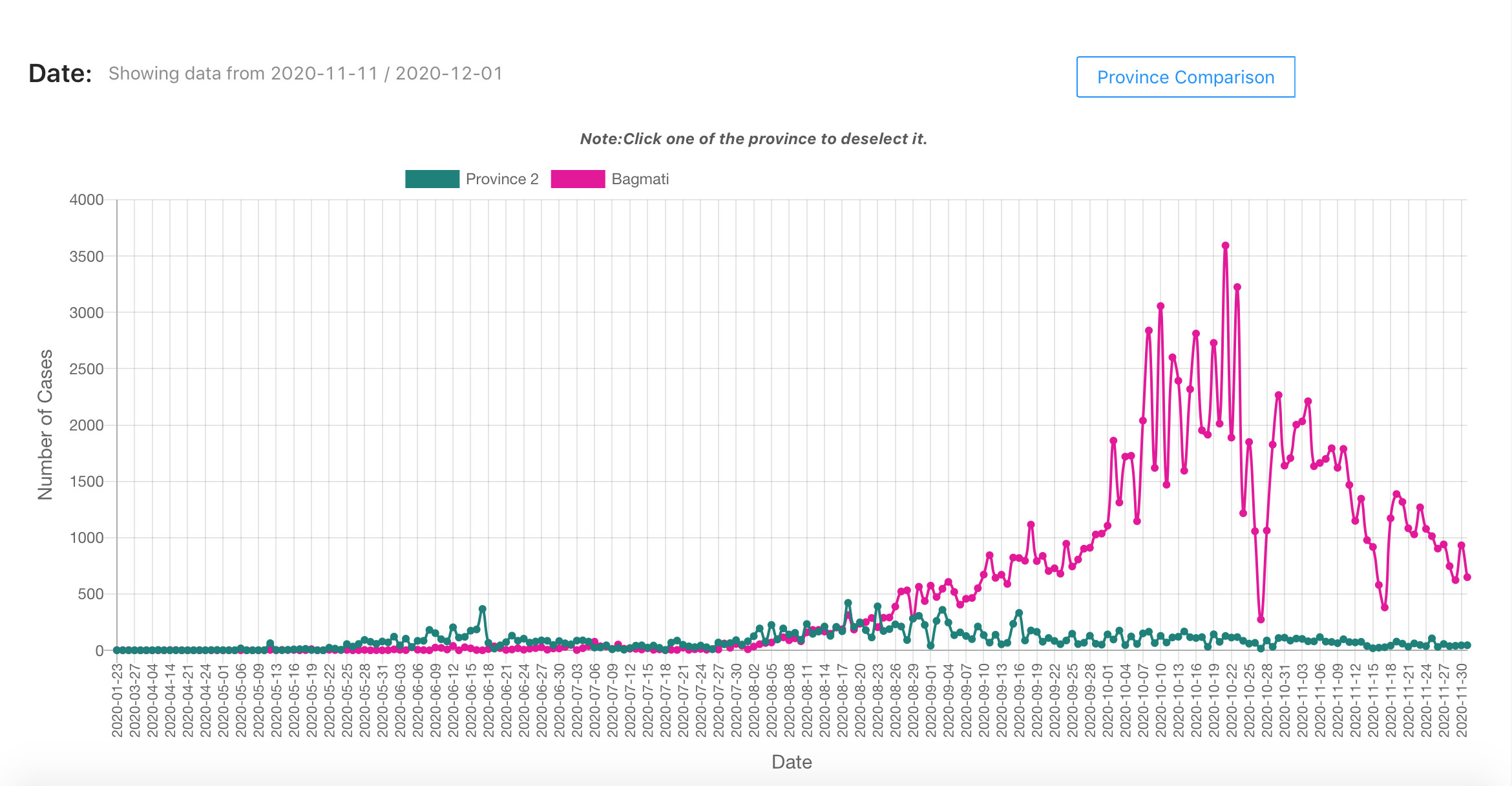
The positivity rate went down, which is a good thing – but it happened for the wrong reason. In October a quarter of people tested came out positive, it is now down to 15% despite the onset of the winter season.
“The risk cannot be underestimated based on numbers of infected people by reducing tests itself at a time when increasingly more people are getting sick or dying of coronavirus,” says infectious diseases specialist Pravat Adhikari. “This argument would be valid only if the infection rate goes down despite an increase in total tests. However, very few tests are being conducted at the moment.”
In fact, such hidden positives lead to more unidentified Covid-19 deaths, adding to the risk. It is reckless of the government to still not launch low-cost PCR tests with quick results, adds Adhikari.
The problem is further exacerbated by unmanaged home isolation, and quarantine cases. According to the Ministry of Health, 10,741 people across seven provinces are self-isolating at home, often without much resources or knowledge on how to manage their condition.
Ideally, asymptomatic or mildly symptomatic people self-isolating at homes should have a separate room and a bathroom. Patients should confine themselves in their rooms, wash their own utensils, wear masks while going to the toilet and sanitise it after use and wipe touch points with disinfectant.
Individuals need to keep track of their temperature and symptoms, measure oxygen saturation level if possible, take paracetamol for body ache and fever and make sure to eat nutritious food. One must be aware of danger signs: oxygen level below 93, chest pain, difficulty in breathing and blue tint to lips and limbs.
But most families who have members in home isolation do not have this information, or live in such crowded quarters that it is impossible to fulfil all precautions. Conflicting directives from the government haven’t helped.
At one point, overwhelmed with the surge of Covid-19 cases in Kathmandu, the Ministry of Health spokesperson Jageswar Gautam advised people live on television to go to hospital only if they feel faint. By then it is too late because it means the patient’s oxygen saturation is already dangerously low.
The government has left the people to their own devices, and ignored expert advice on increasing the number of beds in wards with basic oxygen supply instead of spending money on ICUs and ventilators.
"When I tested positive for coronavirus and had slight difficulty breathing, I called a government health expert for advice, and he himself dissuaded me from going to a public hospital," says Rajendra Dahal, Editor of the magazine Shiskyak. “This is why the death rate is going up, while the positive totals are going down. People are at home, and their oxygen levels are falling, and they have no idea. The main point is that the people have lost their trust in the government health system.”
The chief consultant at the Infectious Diseases Hospital in Teku Anup Bastola agrees that the risk has been heightened because health experts are unaware about the actual condition of people isolating at homes. “Nepalis have a tendency to not visit hospitals until it’s too late. We have found that this is even more true for coronavirus,” he says.
With much of the 2020 overshadowed by the pandemic and its impact on all the sectors, young people wanting to get back to their lives are now ignoring the signs and symptoms, preferring not to voluntarily test in case they might have to isolate for two weeks.
Even according to government figures, the number of people testing positive in Kathmandu Valley is not going down. With the marriage season, and people intermingling indoor in banquet halls, the surge is not expected to subside. At Pashupati Aryaghat, there are five times more cremations happening compared to the same period last year, according to reports. It is not clear how many of these extra deaths are due to Covid-19.
The movement of the younger people has had a direct impact on the elderly, as they take home the virus and make parents and grandparents seriously sick. People in their sixties and above now make up over 60% of Covid-19 fatalities in Nepal.
Even without the added risk of coronavirus, senior citizens are prone to pneumonia and other chronic respiratory illness in winter. Public health experts advise being alert in regards to their condition even before they complain of symptoms and keeping communication channels open.
Says Sher Bahadur Pun: “These are extraordinary times and we need to take extraordinary measures to protect the more vulnerable among us. Until we get a vaccine, we must realise our responsibility in containing the virus and not become a medium for more deaths.”
