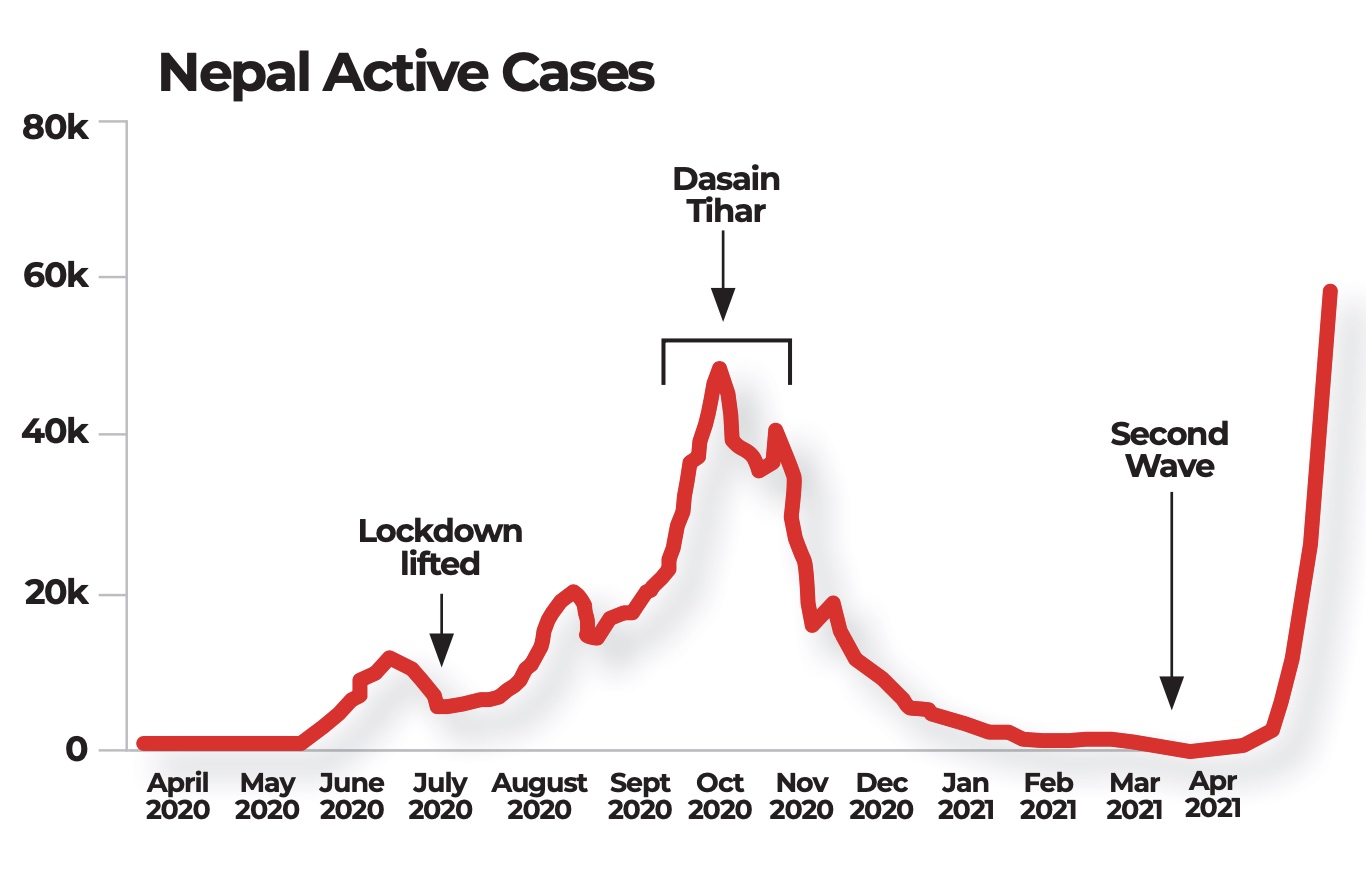
Nepal’s first wave of the coronavirus last year now looks like a ripple, and what the country is now witnessing is the main eruption.
A lot of the attention is on Kathmandu Valley because more than half the daily new Covid-19 cases are here. But it is the Tarai districts bordering India that have been ravaged first, just like last year, but on a much vaster scale.
Epidemiologists say what happens in India arrives in Nepal four weeks later, and the border cities precede Kathmandu by two weeks. Banke district, for example, which is the gateway to Nepal for most returnees from India, is the second most affected after Kathmandu, with 4,811 active cases.
Banke’s positivity rate is shocking: 210 of the 299 PCR tests at Nepalganj Medical College (NMC) in Kohalpur in 24 hours on Tuesday were positive -- 19 times higher than the rate a month earlier.
The doubling time for the infection at Bheri Hospital in Nepalganj is only eight days. The hospital did 1.6% of all the tests nationwide in the past two months, but had 5.35% of the new cases in that time.
One would have thought that the first wave would have prepared Banke and indeed Nepal for this one. But what is happening now is a tsunami.
Last year, when we caught up with Deputy Mayor Uma Thapa Magar of Nepalganj, she was trying to enforce mandatory quarantine on returnees from India, and trying to make sense of a virus that no one knew much about. The mixed directives or inadequate resources from the federal government did not help. Municipalities were left to fend for themselves.
“We were learning as we went along, this time we are dealing with a completely different virus," says Deputy Mayor Magar. "Last year the patient numbers were manageable, even with home isolation. This year, a high share of those who test positive need hospital beds with oxygen. If we cannot provide oxygen, we lose them. There is enough oxygen, but not enough cylinders."
The first wave was a dress rehearsal for the second one. Local leaders have learnt that the border is the chokepoint, and 70% of cases initially were among those with travel history. At the Indian border, health personnel are working in three shifts to screen inbound Nepalis with antigen tests. Those testing negative are kept in holding centres, then transported to home districts by local governments. Positive patients are kept in isolation in Nepalganj, or taken to their domiciles with the support of the Red Cross. These pre-established networks from the first wave have made the work smoother, but the sheer numbers have overwhelmed local capacity.
Bheri Hospital had 140 beds and NMC had 50, which had been expanded to 220 and 300 during the first wave. As our report this week shows, Nepalganj has also added isolation centres, including with oxygen supply, to reduce the pressure on the hospitals. But even with all this, it is not enough.
“We are operating beyond capacity,” says Prakash Bahadur Thapa, the physician who heads Bheri Hospital, sounding fatigued on the phone. “Of the 277 patients now, 180 need oxygen and 9 are on ventilator support, 77 in ICU beds. We are using up to 400 oxygen cylinders daily, before Covid we needed only 10-20 per day.”
More than 100 staff at Bheri Hospital have tested positive. More support has been added, but even doctors and nurses with mild symptoms are caring for patients in the Covid-19 wards. A bed is available only when a patient recovers or dies. Says Thapa, “There is no comparison between the first and the second wave, and the next two months will be difficult.”
The number of deaths is also higher during the current spread, and even the Nepal Army is overwhelmed in management of bodies. We asked Thapa what is most urgently needed. His reply: more hospitals need to be included as Covid-19 facilities. Just two hospitals with limited beds are already inadequate.
Nepalganj shows that local governments are best placed to react urgently to the ground situation. But Deputy Mayor Thapa Magar says the scale of this crisis means that they need help with medical supplies, oxygen, cylinders, setting up more isolation centres. Voluntary organisations can also help by mobilising awareness about using masks and avoiding crowds. The only way to stay alive in the pandemic is not to fall sick in the first place.
Physician Thapa at Bheri Hospital puts it bluntly: “In the coming days, it will be the availability of oxygen that will determine how many live and how many die.”
An exasperated Sunil Singh, chair of Ward 2, says Nepalganj must declare a health emergency. “Imagine if this was an earthquake or a flood disaster, what would our response be? More medical supplies, more health staff, temporary health centres, food rations for the needy. Kathmandu and Karnali Province have not done enough. This is a war. We are hanging by a thread, how much longer before it breaks?
Read also: “Our health system can’t contain the pandemic”, Nepali Times
